Dieting May Slow Your Metabolism – But Weight Loss Is Still Not Futile!

Ever heard that “there is no point in trying to lose weight” because even if you lose weight you’ll gain it back because “your body is fighting you?”
I’ve seen this claim about resting metabolic rate and weight loss so often that I knew it needed investigation:
Is it true? Does dieting slow our metabolism? And if yes, does that make any effort to lose weight futile?
So I turned to the expert, Maeve Hanan, a Specialist Dietitian working in the National Health Service in the UK.
Maeve has written articles for nutrition magazines and runs a blog called “DieteticallySpeaking.com” which promotes evidence-based nutrition messages and dispels nutritional nonsense and fad diets.
Some of her popular posts include her “Nutritional Nonsense Detection Kit” and “A Brief History of Fad Diets.”
After the Biggest Loser weight loss study hit the headlines I asked Maeve to explain to us the relationship between resting metabolic rate and weight loss – and answer the critical question: Is any attempt to lose weight doomed from the start?
(Reveal: science says the answer is no, weight loss is NOT futile and it is worth your attention.)
Let’s hear it from Maeve Hanan.

This is the most packed write up on the subject you’ll ever find in one place, so a table of contents will come handy.
Maria: Let’s start at the start, what do we actually mean by our metabolism?
Maeve: Metabolism means the chemical processes that occur within a living organism in order to maintain life2; and therefore support normal organ functions such as breathing, digesting food, maintaining our temperature, repairing cells etc.
Two terms related to it are basal metabolic rate (BMR) and resting metabolic rate (RMR):
- BMR = the minimum amount of energy (or calories) required to carry out these chemical processes while the body is awake but at rest is called the basal metabolic rate. When we discuss a ‘slow metabolism’ we generally mean a low BMR3.
- RMR = another term very similar to BMR; however RMR is measured under less restrictive conditions than BMR as test subjects don’t need 8 hours of sleep in a test facility prior to measurements6. RMR is generally measured via indirect calorimetry which measures an individual’s carbon dioxide production and oxygen consumption in order to calculate their energy expenditure5.
To avoid confusion between the different names for our metabolic rate I will refer to this as RMR.
Maria: So RMR shows how much energy we need to function when we do nothing, just to be alive. Is it true it accounts for the majority of energy our body needs?
Maeve: Yes it is, our RMR accounts for roughly 60 – 75% of our daily total energy requirements, and the remaining 35 – 40% is composed of the energy which is used for physical activity and thermic effect of food (i.e. the energy the body uses above the RMR due to digesting and store food)5,6.
Maria: Ok, so we need the majority of daily calories just to live – physical activity excluded. My next question is – do some people have faster metabolisms than others? If yes, why?

Maeve: RMR varies between individuals based on a number of factors such as: age, gender, body size, genetics and muscle mass.
For example, as muscle cells require more energy than fat cells to function those with a higher muscle mass generally have a higher RMR; men usually have a higher RMR than women as their body composition has a higher muscle to fat ratio; and as we tend to gain fat and lose muscle mass from roughly the age of 30 onwards our RMR usually decreases in line with this3, 5-8.
Certain medication such as beta-blockers can also reduce an individual’s RMR; as can stopping medications which promote thermogenesis such as: beta-adrenergic drugs, stimulants or nicotine6.
Maria: So the more muscle, the faster our metabolism! Good to know. Let’s discuss resting metabolic rate and weight loss. Can we boost up our metabolism by eating certain foods?

Maeve: Products such as tea, coffee and spices are sometimes promoted to ‘increase your metabolism’, however the evidence to support these claims is weak, and where there is an effect this seems to be marginal and extremely variable between people3.
Maria: I knew there were no “metabolism-boosting” foods! Now let’s turn to hormone levels. Are there any hormones that affect our resting metabolic rate?
Maeve: Yes there are a few actually.
An underactive thyroid which results in the body not producing enough thyroid hormones (i.e. hypothyroidism) or Cushing’s syndrome where a high level of the hormone cortisol is released into the body can both result in a lower RMR3-9; these conditions can both be clearly diagnosed by the way.
The hormone leptin is also thought to affect our RMR as this is involved in regulating our appetite and metabolic processes.
When our fat cells reduce our leptin levels decrease which increases the hunger signals in the hypothalamus in our brain and slows our RMR; on the other hand when our fat levels increase our leptin increases which should reduce hunger signals and increase our RMR12,13.
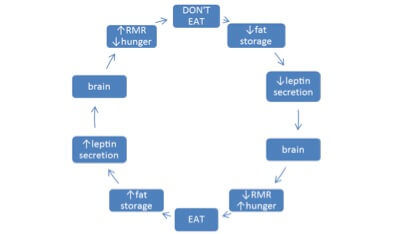
It is thought that people can become resistant to leptin which results in impaired signals from the fat cells to the brain; therefore when fat cell levels increase the consequent reduction in appetite and increase in RMR doesn’t occur as it should, which may increase obesity risk12.
There is a lot of on-going research into this area.
Insulin is another key hormone as it regulates how carbohydrates, protein and fats are metabolised by the body.
Maria: What do we know about resting metabolic rate and weight loss? It seems that weight loss slows down our metabolism…
Maeve: Yes there have been some studies which have found that to be the case, which is often referred to as ‘metabolic adaption’ or ‘adaptive thermogenesis’.
These are very similar terms which basically mean a slowing of RMR as a result of weight loss, which occur above what would be expected when the changes in body composition (as a result of losing weight) are taken into account1.
This adaption is thought to vary significantly between individuals and may partially explain why weight loss plateaus over time and why regaining weight can be common12.
Maria: What about the Biggest Loser study? It showed an interesting relationship between resting metabolic rate and weight loss.

Maeve: Good point, let’s take a look at the findings form “The Biggest Loser” Study.
The study itself measured 14 of the “Biggest Loser” finalists before the competition1, after the 30 week competition and also after 6 years, using DEXA measurements of body composition and indirect calorimetry for RMR.
The aim of the study was to investigate the effects of metabolic adaption, and whether this reduction in RMR was associated with weight regain.
The results of this study found that on average, that 41kg (±31.3 kg) was regained 6 years after the competition, and when the measured changes in body composition and the increased age of the participants were taken into account, the mean RMR was roughly 500 kcal/day lower than expected.
The authors conclude that: “long-term weight loss requires vigilant combat against persistent metabolic adaptation that acts to proportionally counter on-going efforts to reduce body weight.”
Maria: So on average people needed to consumer 500 cal less than normal? Tough! So did every Biggest Loser participant experience the same slowing of RMR?

Maeve: : No they didn’t, those who had lost the most weight by the end of the competition experienced the greatest slowing of RMR when measured after the 30 weeks, and those who maintained the most weight loss after 6 years experienced greater on-going slowing of RMR.
The authors report that this is likely to be a “[metabolic] response to efforts to reduce body weight from its baseline or “set point” value”.
Maria: Since some of them regained part of the weight, are the Biggest Loser partipants success stories or failure stories?
Maeve: I would say that overall they are success stories as despite the substantial weight regain; “The Biggest Loser” participants’ average maintained weight loss was 11.9% (±16.8%), with 57% of participants maintaining more than 10% weight loss, which is better than a lot of similar weight loss interventions.
The authors of this study suggest that this may be due to the large amount of early weight loss experienced during the intervention (I will discuss the evidence to support this below) and the social pressure of maintaining the weight loss due to “the public nature” of the competition.
Maria: Did they only lose fat or did they lose muscle mass too?
Maeve: Interestingly not, as roughly 80% of weight loss was from fat mass and participants managed to mainly preserve their fat-free mass (which includes muscle, bone, organs etc).
This was presumed to be related to the intensive exercise carried out during the intervention, so it seems that in this case the loss of muscle mass (which consequently results in a lower RMR) wasn’t a contributing factor to the reduction in RMR of the participants.
The authors conclude that: “long-term weight loss requires vigilant combat against persistent metabolic adaptation that acts to proportionally counter on-going efforts to reduce body weight.”
Maria: So is the Biggest Loser study to be trusted?
Maeve: It does seem to be a well-designed study overall and it also claims to be “the longest follow-up investigation of the changes in metabolic adaptation and body composition subsequent to weight loss and regain”. However, it is important to keep in mind that:
- the sample size is very small (14 participants) and
- it doesn’t give us a picture of how RMR responds longer than 6 years after substantial weight loss.
Maria: So back to resting metabolic rate and weight loss – how does weight loss affect our metabolism?

Maeve: Looking at other literature, it is reported that a weight reduction of 5 to 10% can reduce RMR by up to 20% for some individuals6.
Similarly, a meta-analysis by Astrup et al. (1999)14 found that subjects who were previously obese and had lost weight had a 3% to 5% lower RMR compared with subjects who had not lost weight.
More recent studies have observed that the reduction in RMR post weight loss persisted for 6 months to 1 year with those who lost weight; however Bosy-Westphal et al. (2013) only found this association with subjects who regained their weight and found no significant correlation between weight regain and metabolic adaption14,15.
A recent study of 17 participants found that resting energy expenditure (i.e. RMR) decreases after weight loss but this stabilizes after a specific cut off point (of 10% weight loss in this study), but non-resting energy expenditure continues to decrease in line with on-going weight loss (as this continued to decrease after subjects experienced 20% weight loss in this study)16.
Maria: So dieting does slow down our metabolism. Curious, do crash diets or other health fads slow our metabolism more than moderate diets?

Maeve: There is contention over whether crash diets can result in a reduced RMR, in some severely calorie restricted diets it is thought that muscle can be broken down to use for energy which lowers muscle mass and hence lowers the individual’s BMR3.
However other research though has not found any disadvantage to rapid weight loss compared with gradual weight loss on the long term maintenance of this17,18.
Some studies have actually found that a higher level of early weight loss was associated with more successful long-term weight loss19,20.
Maria: Will your metabolism slow down more the more weight you lose?
Maeve: There seems to be a lot of conflicting evidence related to this question also.
As mentioned above, ‘The Biggest Loser’ study found a greater reduction in RMR with those who had lost a bigger amount of weight3, whereas other research found that RMR only reduced to a specific cut off point of about 10% weight loss and stabilised after this (although energy expenditure for activity continued to decrease with weight loss which would likely reduce the overall energy burned)16.
If RMR does reduce in line with weight, this would seem to support the 5-10% weight loss target which is often quoted as a “realistic” goal21, as 5-10% weight loss is also associated with significant health benefits such as reducing the risk of heart disease and diabetes22,23 but may also result in a less significant reduction in RMR.
However there is also conflicting evidence as to whether there is a more substantial health benefit from a higher or lower percentage of weight loss24-26.
Maria: Does weight cycling, or yo-yoing, affect our metabolism?

Maeve: The results of small scale intervention trials on the effect of weight cycling (cycles of losing and regaining weight) to changes in RMR have been mixed, with some finding reductions in RMR as a result of weight cycling and others finding no significant changes in RMR27-30.
The evidence base does not support that weight cycling adversely effects metabolism, body composition, energy expenditure or the success of future weight loss efforts; however more large scale evidence in this area is needed.
Maria: Does taking a break from your diet assist you with weight loss?
Maeve: The famous ‘Minnesota semi-starvation experiment’ from 195034 found an on-going reduction of RMR when subjects were experiencing weight regain via controlled re-feeding where subjects could not eat above their previous baseline intake.
However when subjects were allowed to eat freely they consumed significantly more calories than their baseline intake and the reduction in RMR quickly reversed. A more recent study found an increase in RMR when subjects underwent enforced overfeeding after a period of underfeeding and subsequent weight loss and metabolic adaptation35.
Therefore some argue that including weight maintenance periods, ‘diet breaks’ or ‘reverse dieting’ via re-feeding within weight loss programs could result in more sustained weight loss; however more research into this process is needed36,37.
Maria: Ok, so we’ve covered most of the things we need to know about resting metabolic rate and weight loss.
But what about physiological changes? What is really happening to us when our metabolism slows down?
There is a body of evidence which reports that metabolic adaptations is related to a number of physiological processes as a result of weight loss such as37,40:
- A reduction in body tissue which is metabolically active (although metabolic adaption generally continues to occur when this is taken into account)
- Fat cells regulating how well energy is converted in our cells into a form of energy which our body can use
- Hormonal changes including lower levels of leptin which results in a reduced RMR and an increased appetite, therefore promoting weight regain
- Increased hunger signals which could potentially hinder long term calorie restriction
However, other studies report that the physiological basis of metabolic adaption has yet to be fully explained in humans, and there have been a number of limitations related to these studies such as addressing all possible confounding factors including: age, gender, obesity level, stress, inflammation, daily energy expenditure, body composition, and the type of mathematical modelling used for calculations12.
Importantly, some recent research has found no association between leptin and metabolic adaption, which suggests that our knowledge of the physiological reasons for metabolic adaption are still unclear41; Muller 2016 reports that currently “there is no evidence of an effect of leptin on resting energy expenditure in humans”42.
Maria: But when we lose weight we naturally need to consumer fewer calories because we have a smaller body to support. It seems though that weight loss further reduces our metabolism, right?
Yes exactly, metabolic adaption seems to reduce RMR above and beyond what we would expect from the fact that we need less energy to fuel a smaller body.
Maria: Given the (unsettling) relationship between resting metabolic rate and weight loss, does that mean that attempting to lose weight is futile?
 Maeve: No, I wouldn’t say that, as 5-10% weight loss is associated with substantial health benefits (as discussed above)43-44.
Maeve: No, I wouldn’t say that, as 5-10% weight loss is associated with substantial health benefits (as discussed above)43-44.
For example, if we look at the results of “The Biggest Loser Study” on average the contestants maintained >10% weight loss despite the metabolic adaption which seemed to occur3.
(and here’s why losing 10 percent of your body weight is a BIG win.)
A large meta-analysis by Dumbrowski et al. (2014) found that it is possible to maintain small but significant amounts of weight from non-surgical weight loss interventions.
In particular those which combine behavioural interventions with diet and physical activity, or the use of evidence-based pharmacological substances such as Orlistat (although all Orlistat studies also reported an increase in bowel issues form using this).
Other studies have found that roughly 20% of people are successful at long term maintenance of 10% weight loss46.
I think metabolic adaption studies show how important prevention of initial or further weight gain is to reduce any future chance that the body will try to ‘fight to regain’ a higher weight.
Maria: Does it mean that your body will be working against you and make you regain the weight unless you kill yourself in eating less or exercising more?

Maeve: I don’t think that there is enough evidence to say this for definite yet, as there isn’t any gold-standard research such as systematic reviews this specific question, but it does look likely that a person’s RMR drops after weight loss so an extra effort with restricting calories and increasing exercise may be needed.
But this is only one potential piece of the puzzle when it comes to obesity; genetics, psychological issues and social circumstances also play a massive part in whether a person manages to successfully maintain weight loss not just diet and exercise.
Based on the current evidence we also aren’t sure just how long these potential changes to RMR last as the longest study so far has been 6 years.
Maria: So what are the take home messages from all of this?
Maeve: Overall this is a very complex phenomenon and we don’t have all the answers yet, but our understanding is improving.
The mounting evidence supports that a reduction in RMR occurs after weight loss, which is higher than the expected reduction in RMR when we take into consideration the actual weight loss itself; on-going research is exploring the specifics of how this occurs, including the underlying physiological processes.
More large scale research is needed into whether the speed of weight loss or weight cycling hinders future weight loss attempt and there is conflicting research about whether a large or more moderate amount of weight loss is more beneficial to long term health.
In terms of weight loss maintenance, it seems that long term strict efforts to monitor calories consumed versus calories burned may be needed to counteract metabolic adaption, and preserving lean body mass via adequate protein intake and resistance training is likely to prevent further reductions in RMR3,36.
There may also be a potential for ‘diet breaks’ or ‘reverse dieting’ to improve RMR and support weight loss maintenance; but more research is needed into this.
This evidence adds to the complex picture of obesity; and particularly addresses why it can be difficult to maintain weight loss.
This shows that rather than attaching unfounded blame and social stigma to obesity, which only adds to the emotional and psychological challenges of losing weight, we need on-going high quality research to help us to discover how we can best support those who struggle with their weight.
THANK YOU Maeve for this amazing, science-based interview! Folks interested in science-based nutrition, please follow her at DieteticallySpeaking.com!
Now off the readers – have you also heard the claims that there is just no point in losing weight because of the relationship between resting metabolic rate and weight loss?
Have those claims deterred you from even trying to lose weight? Leave a comment below!







fantastic reading.
Thanks Phil!